“Bio-Well 3.0 now available ex stock, Limited Quantity, 1st come 1st Served basis”
Bio-Well GDV Camera for Aura Photography Scan to Read Aura Energy in Andheri, Mumbai. Bio-Well Aura Camera is a most revolutionary GDV technology to measure Aura Energy and Scan Body Chakras. Kirlian Aura Photography by using a specialized BioWell GDV Camera.
Our Products
Bio-Well 3.0

Know your Energy / Chakras Status & also Stress and Health Status
Bio Cor

Balance your Body Energy / Chakras reduce stress, restore calm & alertness.
Sputnik

Know the Positive/Negative energy of a Place, Location, Home, office…
Water sensor

Allows for the testing of water’s response to environmental stimuli…
Glove
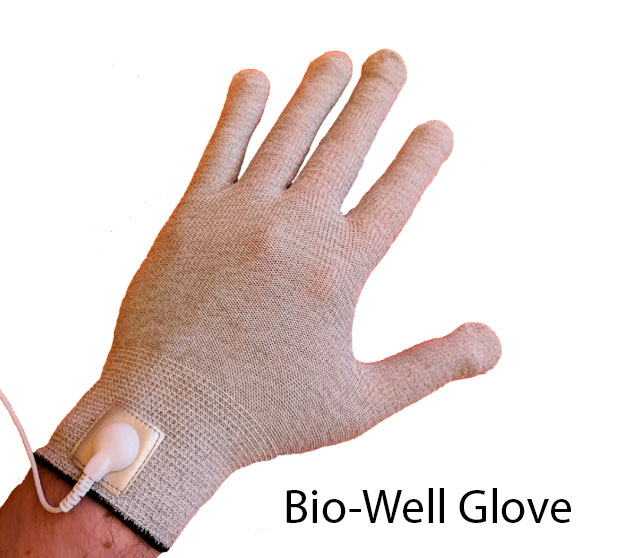
Is Designed for real-time measurements of a person’s stress levels…
We offers Aura Photography Reading or Aura Reading Service in Mumbai. Please phone on +91 70456 98373 for an appointment. Aura Photography Fees – INR 3000/- only (Price Inclusive of Detail Aura Scan Report).
New Products HeartMath Inner Balance™ app/sensor and emWave® Pro Multi-user – HeartMath measures a person’s current stress level and shows the results on a laptop or mobile. It is a powerful technique to monitor stress levels based on your heart rhythm biofeedback.
HeartMath Inner Balance™ app/sensor and emWave® Pro Multi-user Know More
Aura photography is the new trend to Check Your Health Status.
know your health status and stress level
super FAST full body aura scan in 10 min.
get report on Aura energy & chakras
About Us
Dr. J M Shah an Alternative Therapist has introduced GDV Camera the first time in India.
Dr. J M Shah has his specialization in curing heart disease Aura Kirlian Photography, Chakra Balancing, and is also a PhD Degree holder from the University of Colombo in Alternative Medicines.
Dr. J M Shah has brought GDV Camera Technology to India in 2002 and since then , he is continuously working for the well-being of humanity, and for that, he has conducted many seminars, workshops and has participated in events and exhibitions through out India.
Dr J M Shah started Suru Kirlian Photography Center in Andheri, India, Mumbai for Aura Photography Scan Test, Kirlian photography and Aura Report to know Aura Energy and Body Chakras Position Before and After healing Treatment. Suru Kirlian Photography Center received sole Distributorship from Dr. Korotkov of BIO-WELL Company (Russia) for Bio-Well GDV Camera for India. Think about Buying Bio-Well GDV? Bio-Well Camera Now Available in India
Our Wellness Journey Contributor

Dr. Jashvant M Shah
Founder, Charmain & MD Suru Group of Company and Suru Kirlian Photography Center Andheri, Mumbai, India

Dr. Konstantin G. Korotkov
Inventor of Bio-Well GDV Camera and Founder of Bio-Well Company Russia

Aura Photography
Suru Kirlian Photography Center Andheri Mumbai, India provides Aura Photography Scan or Kirlian Photography Services

Bio-Well GDV Device
Authorized Sales, Marketing and Support Partner of Bio-Well Camera or GDV Camera in India

Aura Photography in Mumbai, India | Kirlian Photography by Bio-Well GDV Camera
What Kirlian Aura photography actually represents and what it can be used for. Many acupuncturists, Healers, Therapists, and even many credible Health professionals believe in its diagnostic potential.
Aura photography Camera (Aura reading camera | Kirlian Aura Camera ) captures the aura energy of a person. We Provide Kirlian Aura Photography service in India Mumbai. Aura Kirlian Photography Services is offered by Suru Kirlian Photography Center Andheri East, Mumbai & Get a Report on your Health Status. Our Aura Kirlian Photography Report Benefited to everyone and obtains image reports of Aura Energy of the Human Body, Chakras Position Reports, Health Status Reports, etc…Kirlian Photography cameras are also known as Aura Camera, Bio-Well GDV Camera (Aura Photography camera | Kirlian Aura Camera) will capture the right aura energy field of a person. and that they’ll provide accurate representations of their auras.
Aura is individual energy that surrounds a person’s body. Aura photography is a way to translate person’s auras into the digital world through GDV Bio-Well Camera (Aura Photography camera | Aura Kirlian Camera). With a special aura camera, you can record and display the human electromagnetic energy that originates off a person’s body and transform those readings into an Aura Photography Report.
All the information aura camera collected with the hand fingertips Acupuncture points are fed into the Connected Laptop or Computer. The Aura Photography product consists of a desktop camera and accompanying GDV software. The aura camera itself is designed like a box.
The resulting aura energy images are the informative and noticeable Aura Photography or Kirlian Photography photos you may have seen on the computer. Aura Camera, Aura Photography, or Kirlian Photography often looks like a simple headshot of a person with bright aura energy surrounding them. Aura photography requires some special aura equipment, including an aura camera (Bio-Well GDV Camera). But there’s more to aura photography.
Suru Kirlian Photography Center Andheri East [ Mumbai, India] is an Officially certified service center of Bio-Well Company in India. It authorizes the Suru Kirlian Photography Center, Mumbai to provide full technical support, post sales technical assistance, repair and refurbishing of Bio-Well Camera devices. For normal Allopathic Test, we have to go for many many tests like blood test, X-Ray, MRI, CT Scan, Sonography and many more tests for full body diagnosis. By Bio-Well Camera we can get full body diagnosis in 30 Minutes. We also do Aura Photography and kirlian photography services in Mumbai, India which gives report on Aura, Chakras, Stress health and Wellness. Please contact – 022-67353637 (3 Lines) | jashvant2@gmail.com
Buy Bio-Well Camera GDV ((Bio Well 3.0)
Dr.J M Shah introduced Biowell GDV Camera first time in India. Buy Aura Camera The latest GDV Camera – the Bio-Well 3.0 About GDV Biowell Camera Know More

BioCor Device from Bio-Well
BIOCOR is a unique device that aids in shifting and correcting your aura energy state and balance aura, chakras through high frequencies. Know More
Shop GDV Camera Sputnik
Test the energy of a room, location before, during and after you meditate to see how energy levels of Place change. About Sputnik Sensor Know More
Why select us?
We understand your requirement for Aura Camera & Aura Photography and provide quality Sales Services for Bio-Well Devices.
Only Bio-Well Certify Service Center in India
Suru Kirlian Photography Center is an Officially certified service center of Bio-Well Company in India. It authorizes the Suru Kirlian Photography Center to provide full technical support, post sales technical assistance, repair and refurbishing of Bio-Well Camera devices.
Authorized Distributor & Reseller GDV Bio-Well Camera
Suru Kirlian Photography Center Authorized Representative is comprised of global representatives who are experienced in the operation, training, and support of Bio-Well Camera and GDV products. Interest in purchasing Bio-Well products Get in Touch With Us…..
Aura Photography Service & Provide Bio-Well GDV Camera Since 2002
From the Year 2002 Dr.J M Shah Provide Health and Wellness Products and Aura Kirlian Photography Solutions in India. He has brought this GDV technology in India in 2002 and for that he has conducted many seminars, workshops, events though out in India….
Bio-Well GDV products are warranted for (2) two years from the date of purchase.
Bio-Well Product very convenient, user-friendly and informative for practitioners.
Suru Group Andheri, Mumbai, India is One of the Reputed diversified Organizations in India.
Start your journey with us now
Know More About Bio-Well Camera Price…GDV Camera Cost…Aura Photography Camera Price…Kirlian Camera Price…Biowell GDV Cost…Aura Camera Price….Aura Photography Camera Cost…Kirlian Camera Cost…Aura Camera Cost…Get in Touch – 022-67353637 (3 Lines) | jashvant2@gmail.com
Aura Photography Scan in Andheri, Mumbai India | Kirlian Photography Scanning in Andheri East, Mumbai India | Kirlian Aura photography by Aura Photography camera or Kirlian Camera or Bio Well GDV Camera
Our Blog
check out our Official Blog for the Latest Articles, Product Updates, and News on Biowell GDV, Aura Photography, Kirlian Photography, Aura Camera & Health etc…
Interesting Corner: Few of the Interesting Articles
–How Aura Photography Helps Healers
–The Key To Good Health, Aura Photography Is As Important As The Life Insurance
–The Myth and Science of Kirlian Aura Photography
–Aura Kirlian Photography for Healers, Therapist, Alternative Medicine Doctor Pre and Post treatment
–Future Diseases – Know Your Aura Energy Field Know Future Diseases
12,458+
Aura Photography finished and Completed
110+
Bio-Well GDV Camera
Clients in India
1,000+
Positive Feedbacks for Aura Photography & Bio-Well Camera
210+
Technical support, Repair and refurbishing of Bio-Well 2.0
Russian Bio-well Camera – Get Aura energy field analysis done in 15 minutes to know health problems of your full body. Please phone on +91 7045698373 for appointment. Aura Photography Fees – INR 3000/- only.
Suru Kirlian Photography Center Andheri (East), Mumbai received Sole Distributorship from BIO-WELL Company for Bio-Well GDV Camera and Bio-Well Products in India.
Get in Touch
Know More About Aura Photography, Aura Camera, Bio-Well Camera, GDV Camera, Bio-Well Sputnik, Kirlian Photography Camera, Kirlian Camera & Aura Photography Camera
Know More About Bio-Well Device & Aura Photography
For Inquiry Submit Form
Bio-Well Device & GDV Camera Products

Here for you
Call us: 022-67353637 (3 Lines). Mobile: +91 7045698373 – We are there for your support.
Mail Us
Email: jashvant2@gmail.com For More Detail about Bio-Well GDV Device E-Mail Us Now.
Where to find us
Suru Kirlian Photography Center, 11, Sona Udyog, Andheri (East), Mumbai, India





